
Lessons learned from assessing health facilities with a focus on maternal and child health and using systems thinking in four Sub-Saharan African countries.
How many maternal deaths does a region generate to have 100.000 live-births?
The answer to that question reflects inequalities in access to quality health services. According to UN inter-agency estimates showed that In 2020, sub-Saharan Africa had 545 maternal deaths per 100,000 live births as compared to 223 deaths per 100,000 live-births globally, and only 4 deaths per 100,000 live-births in Australia and New Zealand!
The ALERT project aims to design and test interventions aimed at reducing the Maternal Mortality ratio (MMR) in big hospitals that deliver more than 2500 babies per year in Benin, Malawi, Tanzania, and Uganda. Understanding the functionality and readiness of health facilities to provide high-quality maternal and newborn health services using Health Facility Assessment (HFA) tools is needed in designing effective and context-appropriate quality improvement initiatives. Existing HFA tools available for collecting data related to maternal and newborn care lack aspects that cannot be measured and quantified solely by numbers such as governance and leadership.
The ALERT HFA was designed after reviewing existing HFA tools and adapting these to understand complexities in the provision of maternal and newborn care. The tool applies a system thinking approach and is organized in 17 sections which cover broad dimensions for a more well-rounded assessment including, hospital governance, leadership, financing, human resource, health management information system, monitoring and evaluation, and COVID-19 related adjustments to care. The tool is designed to identify system-wide gaps and design interventions that truly respond to the context and the needs of the stakeholders involved in the provision and utilisation of maternal and newborn care.
The overall goal of this study is to draw lessons from the innovative HFA tool, through in-depth conversations with senior experts who implemented the HFA tool, which could be used to improve similar HFAs. Being collected during the COVID-19 pandemic, the ALERT HFA also reflects facilities’ resilience and response to crises.
The Figure below shows the challenges experienced and opportunities and strategies taken during the HFA implementation.
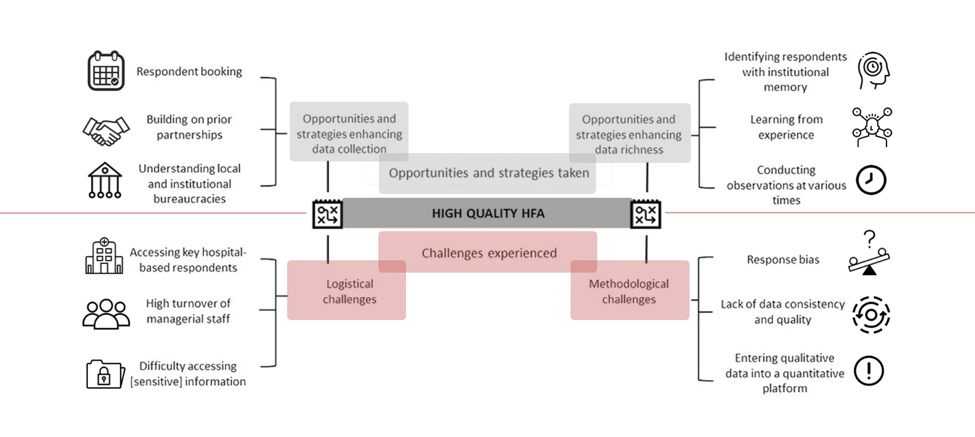
Logistically, the main challenges were accessing the key hospital respondents and the high turnover of managerial staff. Also, sharing difficult accessing sensitive information, such as those on finance and maternal deaths, which needed to be approved by managers, most of whom were reluctant to talk about these topics. As far as the methodological challenges, there were human errors and inconsistencies in keeping the data record. Previous working relationships between some of the HFA interviewers and respondents also created biases toward the topics related to governance, human resources, and quality improvement.
To overcome the mentioned challenges, HFA data collectors implemented the following strategies:
In collecting the data, they capitalized on their experiences of local and institutional bureaucracies, organization cultures, and power dynamics to be able to make the right move. Additionally, HFA data collectors engaged in advance communication and built on their existing partnerships with the hospital staff.
Pertaining to measures taken to enrich the quality of data, HFA data collectors included key respondents (senior staff with long experience in the assessed hospitals and communication officers) in addition to those in managerial positions.
After comparing the sequencing of hospitals for the HFA fieldwork across the teams in the four countries, we found that collecting data from the nearest hospital first and learning from the experience was more efficient as it allowed the teams to revisit the nearest hospital which was assessed first; it would have been harder to do so if they started with the hospitals further away. This way they saved time and gained more quality data.

0 comments